|
Meticulous and systematic examination is essential. Nerve injury and the corresponding loss of muscle strength was found to recover well in all patients 11 therefore surgical exploration of these nerve injuries is rarely recommended.Ī thorough history should be taken, in particular with regards to mechanism of injury, hand dominance, level of function, occupation and past medical history. Nerve lesions were more frequently found in displaced fractures (82%) than undisplaced fractures (59%). They observed that the nerves most frequently involved in descending order were the axillary, suprascapular, radial, musculocutaneous, median, and ulnar nerves. 11 Denervation on the electromyogram was found in 96 of these patients (67%). conducted a study of 143 consecutive proximal Humerus fractures in the setting of low velocity trauma. Neurological injury is more common in open fractures and in the elderly. Despite this, few studies documenting the incidence of neurological injury in proximal Humerus fractures have been published. Nerve injuries are relatively common in Proximal Humerus fractures. 8 Although higher energy fractures and significant soft tissue stripping from the Humeral head may lead to disruption of the arcurate artery, this can occasionally be compensated for by collateral blood supply and AVN is not inevitable. Fractures with short calcar fragments (<8 mm), surgical neck fragments or a disrupted medial hinge can lead to arcurate artery injury and subsequent ischaemia of the proximal Humerus and eventually avascular necrosis (AVN). Direct injury to this artery is exceptionally rare in proximal humeral fracture. The blood supply to the proximal Humerus arises from both the anterior and posterior humeral circumflex branches of the axillary artery. The lesser tuberosity is displaced medially by the subscapularis tendon. The greater tuberosity is distracted by the supraspinatus and teres minor, which produces a posteriosuperior displacing force. In the case of the humeral shaft, the pectoralis major attaches to and distracts it inferiorly and medially. The understanding of the actions of these tendons is key to predicting the deforming forces which lead to the various fracture patterns observed. In 1970, Neer first published his classification of proximal humeral fractures 7 and subdivided the proximal Humerus into 4 parts for ease of interpretation: the humeral head, shaft and both the greater and lesser tuberosities.Įach of these fragments may be displaced by the action of tendons. In light of this evidence, as well as longer term follow up studies supporting the PROFHER trial, 4 the authors would like to distil and clarify existing evidence with the hope of informing the orthopaedic practitioner of the modalities of non-operative treatment and the outcomes that can be expected as a result.ģ. Applied anatomy of the proximal humerus Options for operative fixation have increased in the last two decades, though recent evidence emerging from the PROFHER 3 trial would suggest that non-operative fixation is preferable in these injuries. These fractures present a real challenge for the treating surgeon in terms of accurate diagnosis, classification and treatment.ĭespite the high incidence of these injuries within the population, there remains a comparative lack of high-level evidence available regarding their treatment, in particular with regards to the more complex comminuted fractures of the proximal Humerus. Ultimately, the objective for the treatment of proximal humeral fractures is the restoration of pain free movement and strength in the shoulder. 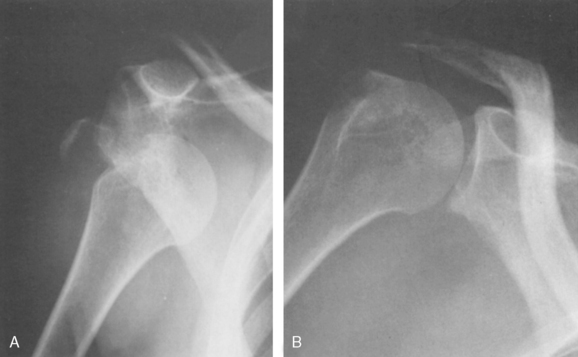
2 These are often debilitating injuries, resulting in significant loss of function, irrespective of their mode of management. 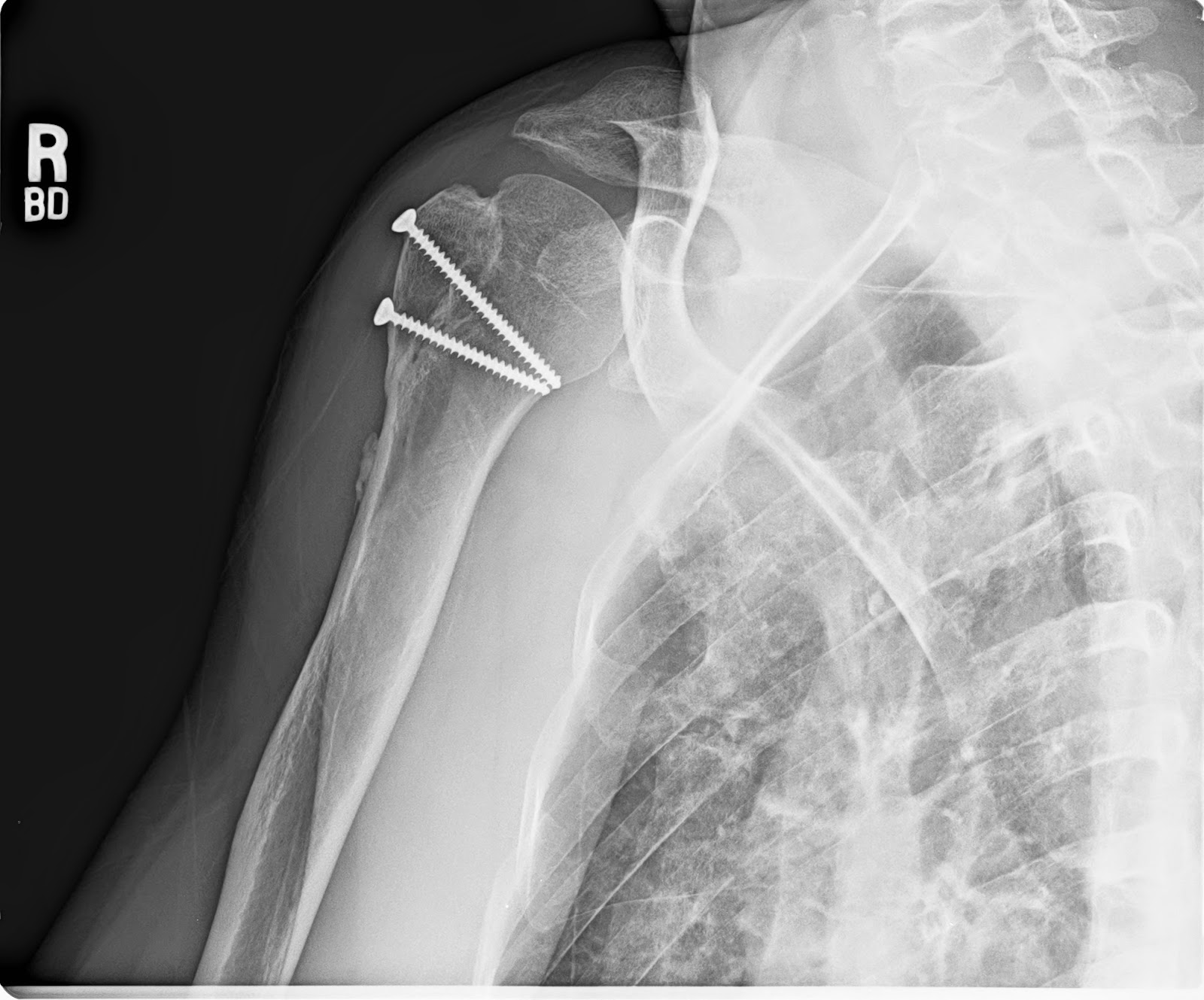
1 They are the third most common type of fracture in the elderly, affecting 250 in every 100000 patients in the United States. Proximal Humerus fractures are increasingly common, comprising 4–5% of all fractures.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
